There is ample research documenting the existence and persistence of mental health and mental health care disparities over the past several decades (1). For example, research consistently suggests that there are racial and ethnic differences in prevalence of some mental disorders (e.g., compared to non-Hispanic Whites, Blacks/African Americans have higher rates of diagnosed schizophrenia [2] and American Indians/Alaska Natives have higher rates of posttraumatic stress disorder [3]). Across diagnostic categories, racial and ethnic minority individuals have more severe and persistent impairment than non-Hispanic White individuals (4, 5). Similarly, compared to cisgender heterosexual individuals, sexual and gender minorities have higher rates of depression symptoms and suicidal behaviors (6). Despite efforts to address mental health and mental health care disparities, there remains a significant gap between our ability to document, investigate, and understand mental health disparities and their causes and to translate this research knowledge into interventions that meaningfully reduce disparities in clinical and health care outcomes.
The National Institute on Minority Health and Health Disparities (NIMHD) Health Disparities Research Framework (hereafter “the framework”) is intended to encourage a comprehensive approach to understanding and addressing health disparities with respect to race/ethnicity, socioeconomic status, sexual and gender minority status, and rural versus urban residence (7, 8). The framework, which is an extension of the socioecological model, consists of two dimensions: domains of influence on health (biological, behavioral, physical and built environment, sociocultural environment, health care system) that occur at different levels of influence on health (individual, interpersonal, community, societal). The individual cells of the framework each represent categories of potential determinants of health disparities and/or intervention targets to address health disparities.
Much of the focus in mental health disparities research, including research supported by the National Institutes of Health (NIH), has been either on single cells of the framework (e.g., individual-level biological determinants), single levels of influence (e.g., individual-level biological and behavioral determinants), or single domains of influence (e.g., lack of access to mental health care as the primary driver of disparities). However, this approach does not take into account the complex interaction of structural and social determinants of mental health that create mental health disparities. Thus, addressing mental health disparities requires research that explores factors at multiple levels of influence, particularly beyond the individual level. Such research should prioritize an understanding of how community, social, and structural factors, including structural racism and discrimination, impact individual-, community-, and population-level mental health outcomes. In addition, research that examines how domains and levels of influence interact across multiple levels (i.e., cell×cell interactions) is necessary to better approximate the real-world complexities of how interconnected determinants impact the mental health of individuals, families, communities, and populations.
To encourage mental health disparities research that uses a multidimensional approach and to provide researchers with a more tailored approach than other existing disparities frameworks and models, we offer an adaptation of the framework specific to mental health disparities (Figure 1). The examples provided within the cells of the framework are intended to be illustrative rather than exhaustive. This adapted framework is similar to other frameworks and models that describe social determinants of health (SDOH), such as those by the U.S. Department of Health and Human Services Healthy People 2030 (9) or the World Health Organization (10). What distinguishes this framework is that it includes both general SDOH and determinants that may be specific to mental health to promote a more comprehensive view of mental health disparities. In addition, the adapted framework emphasizes the simultaneous examination of both domains and levels of influence to provide an organizational structure with which to identify or conceptualize relevant determinants and generate appropriate strategies to address them.
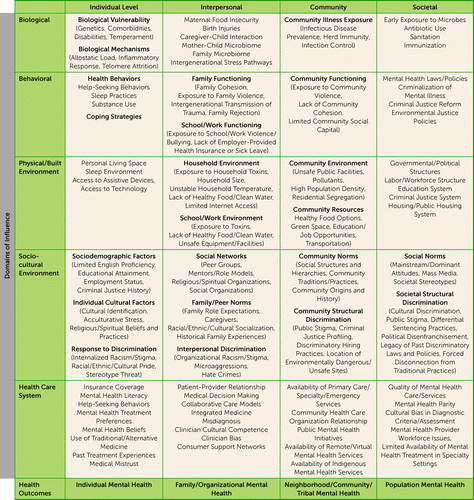
FIGURE 1. An adaptation of the National Institute on Minority Health and Health Disparities Research Framework for mental health disparities
As a hypothetical example, suppose researchers and community partners wish to develop an intervention to improve help-seeking to address high rates of depression and posttraumatic stress disorder in a local Hmong population. The team views health literacy as the key feature driving low levels of help-seeking, but they also identify other relevant determinants, including lack of health insurance, food insecurity, lack of transportation, and lack of availability of Hmong-speaking providers. It becomes clear to the team that a health information–focused intervention alone is unlikely to result in improved help-seeking unless these structural barriers to accessing mental health care are also addressed. We are not suggesting that determinants in all cells of the framework must always be included to address health disparities, but we highlight the importance of examining the constellation of determinants relevant to the specific disparities being studied, and the need to intervene at the appropriate levels to have a sustained impact. The availability of a framework that emphasizes multidomain, multilevel determinants of health does not ensure that research approaches and interventions will successfully address mental health disparities—this depends upon how researchers and stakeholders apply and implement the framework.
Based on the concept of generations of health disparities research (11), we describe examples of three types of mental health disparities research in which the adapted framework may be implemented and that address SDOH. Note that research to document mental health disparities is not included here if does not also examine mechanisms or determinants of those disparities, or if SDOH are measured but included only as control variables in analyses. Although this research progression may be a natural evolution, we argue that the highly incremental research that has characterized much of the health disparities field is not necessary to replicate for mental health disparities, given that this foundational work is often relevant across health conditions and outcomes.
First Generation: Understanding How SDOH Cause, Sustain, or Mitigate Mental Health Disparities
This body of research moves beyond individual-level determinants of mental health disparities (e.g., lack of awareness of mental health problems, lack of health insurance) to identify higher-level social and structural factors that contribute to or mitigate health disparities. Factors such as family and community cohesion, population density, neighborhood-level disadvantage, neighborhood safety and community violence, community social climate, and community and national-level racism and discrimination have all been found to be associated with individual and community-level mental health symptoms and distress (12). This work is critical in identifying modifiable intervention targets that have potential to reduce mental health disparities. Because the social and policy landscape is constantly changing with respect to impacts on minoritized and marginalized populations, this work will always be needed. However, the current distribution, where most mental health disparities research reflects observational research to document and understand disparities, needs to be shifted more toward intervention and action. For example, a recent portfolio analysis conducted by the NIH Office of Disease Prevention of new NIH-funded extramural projects from fiscal year 2012 to 2019 (13) found that about two-thirds of prevention projects were observational, while randomized intervention studies accounted for less than one-fifth of projects, and this proportion declined over time. In addition, only 3.5{e4f787673fbda589a16c4acddca5ba6fa1cbf0bc0eb53f36e5f8309f6ee846cf} of prevention projects included a randomized intervention to address a leading risk factor for death and disability in populations experiencing health disparities. Prevention research specific to mental health outcomes accounted for less than 8{e4f787673fbda589a16c4acddca5ba6fa1cbf0bc0eb53f36e5f8309f6ee846cf} of projects in fiscal year 2019 and mirrored these overall patterns (13).
Second Generation: Evaluating Interventions That Help Individuals Address SDOH or Mitigate Their Impact
This body of research recognizes that the unique experiences of minoritized and marginalized populations need to be acknowledged and addressed in the context of mental health interventions and care. Examples include 1) coping-focused interventions to help individuals manage or reduce distress associated with racism or other forms of discrimination, poverty, unemployment, family separations, and other challenging life circumstances (14, 15); 2) trauma-informed interventions that tailor services for individuals exposed to early or chronic traumatic events or poverty-related stressors (16–18); and 3) patient navigation or service linkage interventions that connect individuals to needed health and social services and/or address access barriers to facilitate engagement in care (19, 20). Such interventions, although a critical component of health and mental health care, only address the consequences of societal inequities and do not directly affect the systems and structures that cause and sustain mental health disparities. In isolation, these interventions will not be sufficient to reduce or eliminate mental disparities at the population level. However, based on our observation of applications submitted to NIH, interventions to help individuals or populations mitigate the impact of SDOH rather than changing the SDOH directly remain common.
Third Generation: Evaluating Interventions That Directly Impact SDOH to Produce Lasting Changes for Communities and Populations
Notably, this area seems to be characterized by more articles calling for social and structural interventions (21, 22) than articles describing the results from actual social and structural interventions (23), and the latter are particularly rare in the mental health field. To address mental health disparities, interventions must move beyond an individual-level treatment-focused model of mental health to emphasize families, organizations, and communities and encompass prevention and sustainable change. Examples of such interventions include medical-legal partnerships in which clinicians and legal personnel work to address discrimination or unfair practices related to housing, education, criminal justice, or other domains (24); alternatives to incarceration for individuals with severe mental illness charged with minor offenses (25); and the implementation of evidence-based depression treatment in faith-based settings (26). However, many structural interventions addressing SDOH have not been rigorously evaluated, and few studies have examined the impact of interventions on disparities (21). Although critically needed, research evaluating these types of interventions has many challenges. Balancing methodological rigor with feasibility and acceptability of study designs can be an issue that requires thoughtful communication and collaboration between research and community collaborators. Studies can be costly to execute, as testing interventions at organizational, neighborhood, or community levels requires these settings to be the unit of analysis rather than the individual, necessitating the inclusion of multiple sites or locations. Interventions addressing SDOH (e.g., racism and discrimination) are likely to have nonspecific outcomes relevant to a range of health conditions, which may pose a challenge to funders who prefer interventions to address disease-specific determinants of health leading to disease-specific outcomes. Despite these many challenges, such interventions hold the greatest promise for eliminating mental health disparities and achieving mental health equity.
On an encouraging note, NIH is beginning to emphasize the need for interventions that move beyond addressing SDOH at the individual level in recent funding opportunity announcements. Topics have included maternal mortality and morbidity (27), structural racism and discrimination (28), family- and community-level interventions (29, 30), physical activity (31), opioid misuse (32), HIV (33), firearm morbidity and mortality (34), and suicide and suicidal ideation and behaviors (35). Although these funding opportunities may include mental health determinants and outcomes, additional targeted opportunities from NIH and other funders of mental health research and services that are explicitly focused on SDOH and mental health disparities are likely needed to make significant progress in this area.
Taken together, this review suggests several important implications for mental health disparities research and clinical practices aimed at reducing disparities. First, this review highlights the opportunity for researchers to use and build upon the proffered mental health disparities framework to mechanistically explore SDOH that can subsequently inform appropriately framed and tailored interventions to reduce disparities. Second, from a clinical perspective, this review points to the importance of establishing a continuum of care to address mental health disparities, which includes both mental health promotion and prevention interventions among marginalized and minoritized populations. Development of interventions aimed at the promotion and prevention end of the mental health continuum of care would facilitate addressing the social and structural factors that have been identified as significant drivers of mental health disparities, including SDOH, and would increase the ultimate reach and range of intervention.
1. : Publications and Reports of the Surgeon General, in Mental Health: Culture, Race, and Ethnicity: A Supplement to Mental Health: A Report of the Surgeon General. Rockville, Md, Substance Abuse and Mental Health Services Administration, 2001Google Scholar
2. : Influence of patient race and ethnicity on clinical assessment in patients with affective disorders. Arch Gen Psychiatry 2012; 69:593–600Crossref, Medline, Google Scholar
3. : American Indian and Alaska Native mental health: diverse perspectives on enduring disparities. Annu Rev Clin Psychol 2012; 8:131–160Crossref, Medline, Google Scholar
4. : Racial/ethnic differences in 12-month prevalence and persistence of mood, anxiety, and substance use disorders: variation by nativity and socioeconomic status. Compr Psychiatry 2019; 89:52–60Crossref, Medline, Google Scholar
5. : Lifetime risk and persistence of psychiatric disorders across ethnic groups in the United States. Psychol Med 2005; 35:317–327Crossref, Medline, Google Scholar
6. : A systematic review of mental disorder, suicide, and deliberate self harm in lesbian, gay, and bisexual people. BMC Psychiatry 2008; 8:70Crossref, Medline, Google Scholar
7. : The National Institute on Minority Health and Health Disparities Research Framework. Am J Public Health 2019; 109:S16–S20Crossref, Medline, Google Scholar
8. : NIMHD Research Framework. 2017. nimhd.nih.gov/researchFrameworkGoogle Scholar
9. . health.gov/healthypeople/objectives-and-data/social-determinants-healthGoogle Scholar
10. : Social determinants of health: overview. www.who.int/health-topics/social-determinants-of-health#tab=tab_1Google Scholar
11. : Toward a fourth generation of disparities research to achieve health equity. Annu Rev Public Health 2011; 32:399–416Crossref, Medline, Google Scholar
12. : Social determinants of mental health: where we are and where we need to go. Curr Psychiatry Rep 2018; 20:95Crossref, Medline, Google Scholar
13. : New NIH primary and secondary prevention research during 2012–2019. Am J Prev Med 2021; 60:e261–e268Crossref, Medline, Google Scholar
14. : Practice recommendations for addressing racism: a content analysis of the counseling psychology literature. J Couns Psychol 2018; 65:669–680Crossref, Medline, Google Scholar
15. : The cultural relevance of mindfulness meditation as a health intervention for African Americans: implications for reducing stress-related health disparities. J Holist Nurs 2014; 32:147–160Crossref, Medline, Google Scholar
16. : Culturally responsive trauma-informed services: a multilevel perspective from practitioners serving Latinx children and families. Community Ment Health J 2021; 57:325–339Crossref, Medline, Google Scholar
17. : Racial and ethnic health disparities and trauma-informed care for children exposed to community violence. Pediatr Ann 2017; 46:e377–e381Crossref, Medline, Google Scholar
18. : Effects of ParentCorps in prekindergarten on child mental health and academic performance: follow-up of a randomized clinical trial through 8 years of age. JAMA Pediatr 2016; 170:1149–1155Crossref, Medline, Google Scholar
19. : Mobilizing community health workers to address mental health disparities for underserved populations: a systematic review. Adm Policy Ment Health 2018; 45:195–211Crossref, Medline, Google Scholar
20. : Does integrated behavioral health care reduce mental health disparities for Latinos? Initial findings. J Lat Psychol 2014; 2:37–53Crossref, Medline, Google Scholar
21. : Structural interventions to reduce and eliminate health disparities. Am J Public Health 2019; 109:S72–S78Crossref, Medline, Google Scholar
22. : Addressing the social determinants of mental health: if not now, when? If not us, who? Psychiatr Serv 2018; 69:844–846Link, Google Scholar
23. : Evaluating strategies for reducing health disparities by addressing the social determinants of health. Health Aff (Millwood) 2016; 35:1416–1423Crossref, Medline, Google Scholar
24. : The medical-legal partnership approach to teaching social determinants of health and structural competency in residency programs. Acad Med 2017; 92:292–298Crossref, Medline, Google Scholar
25. : Community interventions to promote mental health and social equity. Curr Psychiatry Rep 2019; 21:35Crossref, Medline, Google Scholar
26. : Partnering with African American churches to create a community coalition for mental health. Ethn Dis 2018; 28:467–474Crossref, Medline, Google Scholar
27. : RFA-MD-20-008, Addressing Racial Disparities in Maternal Mortality and Morbidity (R01 Clinical Trial Optional). 2020. grants.nih.gov/grants/guide/rfa-files/RFA-MD-20-008.htmlGoogle Scholar
28. : RFA-MD-21-004, Understanding and Addressing the Impact of Structural Racism and Discrimination on Minority Health and Health Disparities (R01 Clinical Trial Optional). 2021. grants.nih.gov/grants/guide/rfa-files/rfa-md-21-004.htmlGoogle Scholar
29. : PAR-21-358, Risk and Protective Factors of Family Health and Family Level Interventions (R01 Clinical Trial Optional). 2021. grants.nih.gov/grants/guide/pa-files/PAR-21-358.htmlGoogle Scholar
30. : RFA-MD-22-007, Community Level Interventions to Improve Minority Health and Reduce Health Disparities (R01 Clinical Trial Optional). 2022. grants.nih.gov/grants/guide/rfa-files/RFA-MD-22-007.htmlGoogle Scholar
31. : NOT-OD-21-087, Notice of Special Interest (NOSI): Developing and Testing Multilevel Physical Activity Interventions to Improve Health and Well-Being. 2021. grants.nih.gov/grants/guide/notice-files/NOT-OD-21-087.htmlGoogle Scholar
32. : RFA-DA-22-036, NIH HEAL Initiative: Preventing Opioid Misuse and Co-Occurring Conditions by Intervening on Social Determinants (R01 Clinical Trials Optional). 2021. grants.nih.gov/grants/guide/rfa-files/RFA-DA-22-036.htmlGoogle Scholar
33. : NOT-MD-21-014, Notice of Special Interest (NOSI): Multi-Level HIV Prevention Interventions for Individuals at the Highest Risk of HIV Infection. 2021. grants.nih.gov/grants/guide/notice-files/NOT-MD-21-014.htmlGoogle Scholar
34. : NOT-OD-21-059, Notice of Intent to Publish Funding Opportunity Announcements for Research on Firearm Injury and Mortality Prevention. 2022. grants.nih.gov/grants/guide/notice-files/NOT-OD-21-059.htmlGoogle Scholar
35. : RFA-MH-21-187, Systems-Level Risk Detection and Interventions to Reduce Suicide, Ideation, and Behaviors in Youth From Underserved Populations (R01 Clinical Trial Optional). 2021. grants.nih.gov/grants/guide/rfa-files/RFA-MH-21-187.htmlGoogle Scholar


